|
Sendblaster torrent. SendBlaster Pro 3.1.6 Multilingual + Keygen. The Tr.im team has removed this link for your safety. We (Tr.im team) work to make sure all our stakeholders adhere to. SendBlaster Pro Edition 4.1.3 Multilingual. Sendblaster 3.1.6 Pro Full Serial Number is a powerful software package program that enables you to. Mar 10, 2015 SendBlaster Pro 4 Full funcionando 2016 - Duration: 4:13. Pirata Pepe 24,265 views. Kevin Mitnick demonstrates how easy it is for a hacker read your email messages - Duration: 6:40.
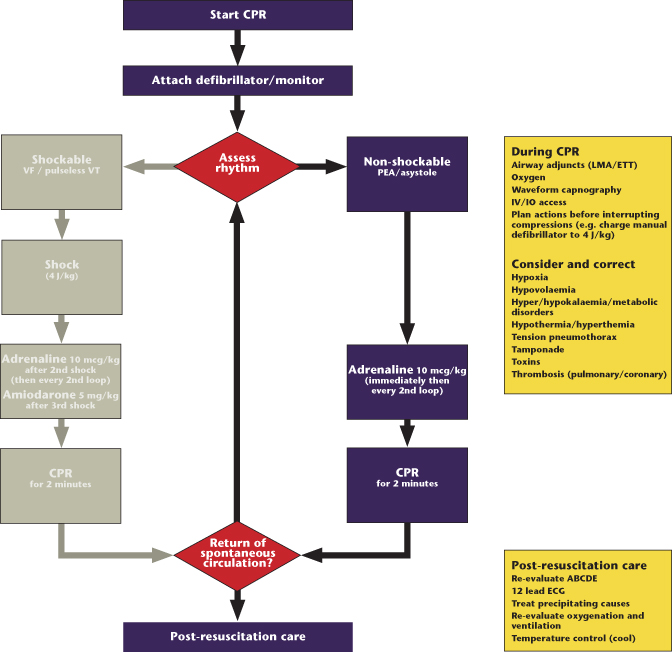
-[Voiceover] Ventricularasystole and pulseless electrical activity are twotypes of cardiac arrest, meaning the heart has stopped. In both of these, a patientdoesn't have a pulse, meaning that they're not pumping blood to the rest of the body, andthat's why both of these conditions are absolutely fatal unless they're corrected immediately. So in ventricular asystole, there's no electricalactivity in the heart. That there's no electricalactivity, that means that the ventricle wallsaren't contracting. And that's what asystole basically means. A means no, and systole implies ventricular contractions. So no ventricular contractions. Again, no electrical activity means no ventricular contractions, means no cardiac output,or in other words, there's no blood flowingto the rest of the body. So there's no cardiac output. And without cardiac output, you're not going to have a pulse. So anybody who has ventricular asystole will not have a pulse. On an EKG, this looks like a flat line because there's no electrical activity to cause any movement on an EKG. And this is the flatline that you hear about on movies and TV shoes, and they say, 'The patient's flatlining!' It's asystole. And then there's pulselesselectrical activity. And this is known as PEA. In PEA, there iselectrical activity on EKG. However, it doesn't result in a pulse. And the electricalactivity you see on an EKG could be something thatnormally produces a pulse, such as normal sinusrhythm, or even heart block, or sinus bradycardia, but for some reason there's not a pulse. Now how could this be? Well, in a normal heart, the heart's electrical activity causes the muscle cells to contract. So you have actionpotentials that propagate or went through the heart, and they'll lead to muscle contraction. And this relationship between electrical activity and mechanical contraction is called electro-mechanical coupling. However, when the heart is under extreme stress, so say the heart'sbeen deprived of oxygen for a long time, thesystem gets disconnected. So, even though there'selectrical activity, it's not going to lead to contractions. Because we've disconnectedthe system, and this is called electro-mechanical uncoupling. So despite the fact that cells can undergo and propagate action potentials, the action potentials don't result in muscle contraction. Another reason why youcould have electrical activity without a pulse is because there could be something blocking the heart. Now the heart has a sac outlining it called the pericardium. And in some cases, thismight be full of blood. And if it is full ofblood, it's going to press down on the heart, andthe heart is not going to have any room to pump. This is called tamponade,or cardiac tamponade. And again, this is thecondition where the heart is constricted by this fluidfilled sac around the heart, and the heart can't pump. So even though you canhave action potentials and electrical activity in the heart, you're not going to be able to pump, and you won't have a pulse. Okay, so I'm sure you've seen in movies or TV shows,when someone flat lines or has asystole, andsomeone else comes running into the room, puts paddles on the chest, and yells, 'Clear!' In this case, they'redefibrillating the patient, meaning they're providing electrical shock to the heart, hopefullyto convert the heart back to a normal rhythm. However, this is a common misconception. We never shock asystoleor PEA for that matter. Defibrillation only works on very specific abnormal cardiac rhythms that can potentially be reversedwith an electric shock, and these are called shockable rhythms. Shockable rhythms includeventricular fibrillation, where the walls of theventricles are spasming, and therefore they can't contract, and they're not going to circulate blood to the rest of the body, and pulseless ventricular tachycardia, meaning that there's some sort of abnormal conduction in the ventricles that cause the ventricles to pump at a dangerously high rate. So neither of these has a pulse. And just a side note, we never shock anyone with a pulse. Something else to note is that even though ventricular fibrillationand pulseless v tach meet the criteria for PEA,and that there's electrical activity but no pulse, we don't typically classify them as PEA. These two arrhythmiasare a class of their own because we treat them differently. They're shockable rhythms. PEA is considered electricactivity without a pulse. That's not v fib or pulseless v tach. Now how do we treat asystole and PEA? Asystole and PEA areconsidered nonshockable rhythms, meaning providing a shock won't likely restore a normal rhythm. How do we treat nonshockable rhythms? We start with cardiopulmonaryresuscitation, or CPR, where we alternate chestcompressions with some sort of artificialbreathing for the patient, whether that be mouth-to-mouth, or doing oxygen through some sort of mask. We'll also administervasoconstrictive medications. Now, vasoconstrictive meansthat we're constricting the vasos, or the vessels. So these drugs constrictthe blood vessels. And equally importantwith any patient who is pulseless, we have to consider any factors that could be reversed that might be contributing to the cardiac arrest. And you can remember which factors to consider by the mnemonic Hs and Ts, which we're going to goover in just one second. So what are the Hs and Ts? Remember, they're potentiallyreversible conditions that could be causing or even contributing to the cardiac arrest. So, if any patient incardiac arrest has any of these factors, we wantto try to reverse it, or fix it, to help save them. Now, something to noteis that a lot of these Hs and Ts are conditionswhere there's some sort of lack of adequate bloodcirculating through the body, or adequate oxygen delivery to the body, including the heart. Heart cells need oxygento function properly. So if there's not enoughoxygen getting to the heart, then the heart cells aren't happy, and they quit working properly. The first H we're going to talk about is hypovolemia, so hypo means low, and volemia refers to volume. So this basically means low blood volume. Usually, from excessive bleeding. In hypovolemia, not enoughblood is circulating, so not enough oxygen is getting around. The next H is hypoxia. That means that there's inadequate oxygen supplied to the body. And hypoxia can be due to many things, such as drowning or even a heart attack. So there's inadequateoxygen getting to the body, to the heart, and to the brain. The next H is hydrogen ions. And hydrogen ionsbasically means acidosis, meaning that the body's PH is too low. And acidosis often results from long periods of hypoxia. We also need to considera person's potassium level, because hypo and hyperkalemia can lead to cardiac arrest. Now, hypokalemia means that there's too low potassium, and hyperkalemia means the potassium level is too high. Potassium plays a reallyimportant role in maintaining normal electrical conduction in the heart. So you can imagine thatif the levels are too high or too low, this will disrupt the heart's electrical conduction system. In anyone with cardiacarrest that comes in, we're going to check their glucose level, because hypoglycemia,or low blood glucose, can lead to cardiac arrest, and this is something that's easily fixed. And the last H we'regoing to talk about is hypothermia, or low body temperature. And typically, we thinkof hypothermia as a temperature less than95 degrees Fahrenheit or 35 degrees Celsius. So as a person's core temperature drops, the heart's pacemakercells fire less and less, and eventually, the heart can stop. Okay, so those are the Hs. Now, let's move on to the Ts. We need to consider toxins, and toxins include bothprescription medications and street drugs. If someone comes inbecause of cardiac arrest due to a toxin, theremight be a reversible agent that will help reversethe effects of the toxins, and can help save the patient. The second T is tamponade, and that's something we just talked about. And we're referring to cardiac tamponade. Like we said, this isa condition where blood fills the space that lines the heart, or the pericardial sac, andthis constricts the heart and makes it a lot harderfor the heart to pump, and sometimes the heartcan't even pump at all. And if the heart's notpumping, no blood circulating. And one way I like to think about it is to think about doing a jumping jack. Now, imagine doing thatjumping jack underwater. It's a lot harder to doa jumping jack underwater because all this pressure's around your arms and legs. Likewise, it's harder forthe heart to pump with all the added pressure surrounding it. And the next T is something called tension pneumothorax. So in the chest wall, the lungs are surrounded by a plural lining. So there's a space createdcalled the plural space between the lungs and the chest wall. In a tension pneumothorax, air can somehow enter this plural space. And this is usually because of some sort of trauma to the chest. And what happens is, airenters this plural space, but it can't leave, andas more and more air enters the space, it crushes the lung, and even pushes the lungand the heart to the side. A crushed or collapsedlung is not going to be able to move oxygen very easily, and the heart can stop. And the last T we're going to talk about is thrombosis,basically meaning blood clot. In the case of cardiac arrest, we're concerned about a blood clot to the coronary artery, or an artery that supplies the heart with oxygenated blood, or we're concerned abouta clot in the lungs, and that's known as a pulmonary embolism. So a pulmonary embolismis a clot in the lung. So clots in either the heart or the lungs can lead to severe oxygen depletion, and eventually lead to cardiac arrest.
• Pulseless electrical activity (PEA), also known as electromechanical dissociation, refers to cardiac arrest in which the electrocardiogram shows a heart rhythm that should produce a pulse, but does not. And the electrical activity you see on an EKG could be something that normally produces a pulse, such as normal sinus rhythm, or even heart block, or sinus bradycardia, but for some reason there's not a pulse. There are 4 rhythms that are seen with pulseless cardiac arrest. They each will be reviewed throughout this section of the course guide. Vfib and pulseless VT indicate electrical activity in the heart and as such can be treated with the hopes of conversion to an organized electrical impulse and rhythm.
Pulseless electrical activity (PEA), refers to cardiac arrest in which the electrocardiogram shows a heart rhythm that should produce a pulse, but does not. Pulseless electrical activity is found initially in about 55% of people in cardiac arrest.[1]
Under normal circumstances, electrical activation of muscle cells precedes mechanical contraction of the heart (known as electromechanical coupling). In PEA, there is electrical activity, but the heart either does not contract or there are other reasons this results in an insufficient cardiac output to generate a pulse and supply blood to the organs.[2]Download free as400 tutorial for beginners pdf reader. While PEA is classified as a form of cardiac arrest, significant cardiac output may still be present which may be determined and best visualized by bedside ultrasound.
Cardiopulmonary resuscitation (CPR) is the first treatment for PEA, while potential underlying causes are identified and treated. The medication epinephrine may be administered.[2] Survival is about 20%.[1]
Signs and symptoms[edit]
Pulseless electrical activity leads to a loss of cardiac output, and the blood supply to the brain is interrupted. As a result, PEA is usually noticed when a person loses consciousness and stops breathing spontaneously. This is confirmed by examining the airway for obstruction, observing the chest for respiratory movement, and feeling the pulse (usually at the carotid artery) for a period of 10 seconds.[2]
Causes[edit]Lidocaine For Pulseless Electrical Activity
These possible causes are remembered as the 6 Hs and the 6 Ts.[3][4][5] See Hs and Ts
The possible mechanisms by which the above conditions can cause pulseless in PEA or the same as those recognized as producing circulatory shock states. These are (1) impairment of cardiac filling, (2) impaired pumping effectiveness of the heart, (3) circulatory obstruction and (4) pathological vasodilation causing loss of vascular resistance and excess capacitance. More than one mechanism may be involved in any given case.[citation needed]
 Diagnosis[edit]
Pulseless electrical activity, it is possible to observe by invasive blood pressure (red) the transition from a normal mechanical activity of the heart, which progressively changes in rhythm and contractile quality to asystolia, even in the presence of normal electrical activity (green), also confirmed by the pulse oximeter detection even if with artifacts (blue)

The absence of a pulse confirms a clinical diagnosis of cardiac arrest, but PEA can only be distinguished from other causes of cardiac arrest with a device capable of electrocardiography (ECG/EKG). In PEA, there is organised or semi-organised electrical activity in the heart as opposed to asystole (flatline) or to the disorganised electrical activity of either ventricular fibrillation or ventricular tachycardia.[2]
Treatment[edit]
Cardiac resuscitation guidelines (ACLS/BCLS) advise that Cardiopulmonary resuscitation should be initiated promptly to maintain cardiac output until the PEA can be corrected. The approach in treatment of PEA is to treat the underlying cause, if known (e.g. relieving a tension pneumothorax). Where an underlying cause for PEA cannot be determined and/or reversed, the treatment of pulseless electrical activity is similar to that for asystole.[2] There is no evidence that external cardiac compression can increase cardiac output in any of the many scenarios of PEA, such as hemorrhage, in which impairment of cardiac filling is the underlying mechanism producing loss of a detectable pulse.[citation needed]
A priority in resuscitation is placement of an intravenous or intraosseous line for administration of medications. The mainstay of drug therapy for PEA is epinephrine (adrenaline) 1 mg every 3–5 minutes. Although previously the use of atropine was recommended in the treatment of PEA/asystole, this recommendation was withdrawn in 2010 by the American Heart Association due to lack of evidence for therapeutic benefit.[2] Epinephrine too has a limited evidence base, and it is recommended on the basis of its mechanism of action.
Sodium bicarbonate 1meq per kilogram may be considered in this rhythm as well, although there is little evidence to support this practice. Its routine use is not recommended for patients in this context, except in special situations (e.g. preexisting metabolic acidosis, hyperkalemia, tricyclic antidepressant overdose).[2]
All of these drugs should be administered along with appropriate CPR techniques. Defibrillators cannot be used to correct this rhythm, as the problem lies in the response of the myocardial tissue to electrical impulses.
References[edit]
Dopamine For Pulseless Electrical Activity Rhythm DiagramExternal links[edit]
Dopamine For Pulseless Electrical Activity Rhythm Strip
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Pulseless_electrical_activity&oldid=900316146'
Comments are closed.
|
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
|||||||||||
- Blog
- Home
- Trek Cc Ryder Bike Trailer Manual
- Erlend Loe Naiv Super Lydbok Nedlastings
- Vir2 Electri6ity Keygen Photoshop
- Tales Of Symphonia Ratatosk Isotoner
- Mashed Drive To Survive Pc Torrent
- Mala Jau De 3gp Video Song Free Download
- Kari 4 Pro With Keygen
- Visual Nastran 2004 Serial
- Download Os X Mountain Lion Installer App
- Sony Xperia Sola Live Wallpapers Free Download
- Atomic Vba Password Recovery Serial Key
- Vusbbus Sys X32 Behringer
- Download Film Punk In Love Full Movie Mp4
- Fable 3 Dlc Download
- Easy Driver Pack Full Crack
- Descargar Crack Para Motogp 2008
- Download Facebook For Bb 9360 Installer
- Collective Intelligence Toby Segaran Pdf
- Acer Navarro Motherboard Drivers
- Civ V Firetuner Youtube
- Screensaver Bergerak Untuk Pc World
- Cd Roller License Key
- Jasc Paint Shop Pro 10 Crack
- Download Free Jumpstart Reading With Karaoke Bars
- The Maze Runner Full Movie In Hindi Hd Free Download
- Sojourn R A Salvatore Epub
- Sherlock Holmes And The Baker Street Irregulars Full Movie
- Windows Phone Xap File Decompiler Java
- Remix Serial Star One Watch Online
- Free Adobe Livecycle Designer Download
- Power Step Plus User Manual
- Ricardo Bacchelli Il Mulino Del Po Ebook Store
- Download Sekirei S3 Full
- Dumitru Constantin Dulcan In Cautarea Sensului Pierdut Pdf
- All Vector Eps File
- Panasonic Md10000 Usb Driver
- Aurora 3d Animation Maker Version 11 Crack
- Beyblade All Episodes Free Download Torrent
- Wayang Jangan Kau Pergi Original
- Encore Electronics Drivers N150mj
- Microsoft Office Picture Manager Editing Marks
- Statistics Freedman 4th Edition Pdf Download
- Bouken Jidai Katsugeki Goemon Ps2 Iso Emulator
 RSS Feed
RSS Feed
